Breast Surgery & Treatment
We offer a multi-disciplinary approach to breast cancer with comprehensive breast and general surgical procedures. Our surgeons are passionate about providing compassionate care as well as educating the community on early detection, diagnosis, and treatment options available for breast disorders.

Breast Disorder Diagnosis
While there are many breast disorders, most are benign (non-cancerous). Treatment options may vary depending on the type of breast disorder that you have. In some instances, a growth or lump may require surgery. However, many breast disorders do not require treatment or surgery. One of the best ways to stay ahead of breast disorders is to have an annual mammogram and an examination by your physician.
We provide ultrasound evaluations and breast biopsy methods including core needle biopsy, stereotactic core biopsy, ultrasound-guided biopsy, and fine needle aspiration, all of which can be conveniently performed in our offices.

Breast Disorder Treatment
Our surgeons create a personalized treatment plan for each patient, offering the most cutting-edge procedures, such as the minimally invasive hidden scar approach. Our team is also proud to offer traditional surgical options. We offer our support through counseling and discuss surgical alternatives in length prior to any surgery.
In addition to offering a full spectrum of breast disease care, our team of highly skilled surgeons specializes in an array of general surgery procedures including open and laparoscopic hernia repair, gastrointestinal procedures, and the treatment of skin and soft tissue disorders.
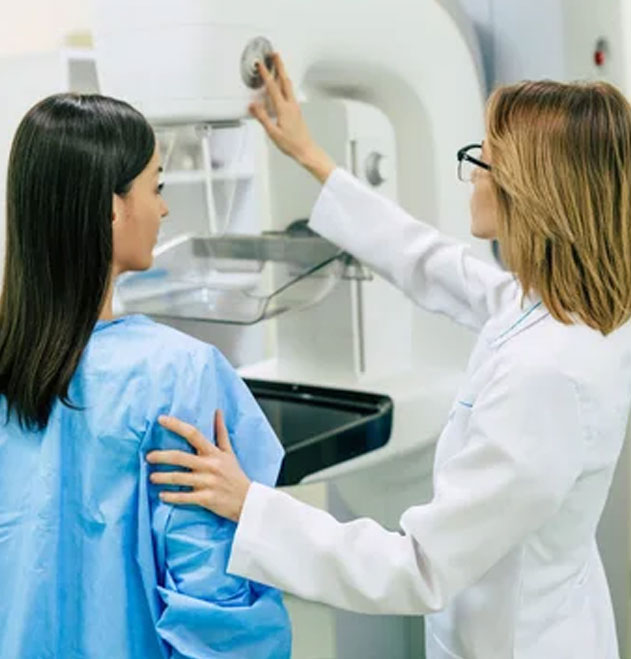
Find Out if Our Breast Surgery Procedure is Right For You
Call 844-973-0002 or fill out the form and we’ll be in touch to answer all of your questions and get you more information. We offer same and next-day appointments for your peace of mind.

Common Benign and Malignant Breast Disorders
If you have been diagnosed with or suspect the occurrence of the following disorders, our specialists can help you get the right treatment and be on the way to recovery. Get in touch with our care team today.
Breast pain & tenderness
The most common type of breast pain occurs during a woman’s menstrual cycle when the breast tissue becomes swollen. Other causes of breast pain include injury, infection, or cysts. If you feel you have a suspicious lump or mass on your breast, it’s important to get it looked at by a physician. Your doctor will determine whether it needs further testing.

Fat necrosis
Fat necrosis occurs when painless lumps form in the breast tissue. Fat necrosis is caused by damage to the fatty tissues and may occur after a lumpectomy and/or radiation from a previous cancerous lump. Fat necrosis can also be caused by trauma to the breast tissue. These lumps are benign and do not increase your risk of cancer. Your doctor may want to perform a mammogram before deciding whether to remove it.

Generalized breast lumpiness
It is believed that most breast lumpiness is caused by normal breast changes in women. If you have lumpy breasts, it’s important to schedule regular check-ups with your doctor and perform regular breast self-examinations, as well as get regular mammograms.
Fibroadenomas
Fibroadenomas are benign, painless lumps. They may vary in size and can be found anywhere in the breast tissue.
Gynecomastia
Gynecomastia is an enlargement of breast tissue seen in male patients. Often, it is caused by high levels of estrogen, or testosterone and estrogen levels that are unbalanced.

Sclerosing adenosis
This breast condition involves an excessive amount of tissue growing in the breast and pain may occur as a result.

Cysts
A cyst, which can feel soft or hard to the touch, is a fluid-filled sac that develops in the breast tissue. Most cysts are benign (non-cancerous) but a cyst aspiration can be completed to relieve tenderness or to rule out cancer.
Uneven breast size
While this is common, especially during the early phases of breast development, your doctor can perform an examination for any mass, abscess, or cyst in the breast.

Hard lump
If you detect a lump that is hard, unmovable, attached to your chest wall, or if you are experiencing dimpling or puckering of the breast, it is important to consult your doctor for further examination.
Learn More About Our Treatments
Breast Biopsies
Breast Biopsies - What You Need To Know
Breast Cancer
Breast Cancer: Diagnosis, Treatment, and Recovery - Dr. Lisa Iucci
Dr. Lisa Iucci
Meet Dr. Lisa Iucci - Breast and General Surgeon
Dr. Desiree D'Angelo
Meet Dr. Desiree D'Angelo - Breast and General Surgeon
Dr. Yolanda Tammaro
My Diagnosis with Triple Negative Invasive Ductal Carcinoma
Dr. Stephen Chagares
Lumpectomy vs. Mastectomy: How Do You Choose?
About the Premier Surgical Network
Healing breast disorders and breast cancer require proper expertise and compassionate care. Your fight to get better is one we take to heart. All of our surgeons are committed to providing our patients with a warm and welcoming environment and offer their support every step of the way from diagnosis to remission.
We are passionate about delivering individualized guidance and emotional support to each patient during the different stages of their breast cancer journey. We have a deep understanding of our patient’s journeys and we advocate for their physical and emotional well-being all the way through.

What Our Patients Say About Us
-Patient review, Healthgrades
Dr. Frost is definitely one of my favorite doctors. He is very knowledgeable & nice. I am very lucky to have found him.
-Patient review, Facebook
Dr. Chuang is great! Highly recommend if you need a breast surgeon.
-Patient review, Healthgrades
I followed Dr. D'Angelo from her previous practice because she is so good. A true professional and a down to earth physician.
-Patient review, Healthgrades
Dr. Frost is very kind. He is a wonderful doctor and always treats me with respect. I would recommend him one hundred percent!
-Patient review, Healthgrades
ER doctors referred me to Dr. Frost. He was compassionate, kind, and understanding. He figured out what the problem was and put me on a path to recovery that has been successful to the point where the results are unbelievable. I would recommend him to the world!
12 Conveniently Located Offices Across New Jersey
Our Specialized Surgeons

Dr. Anjeanette T. Brown
MD, FACS, Physician
Dr. Anjeanette Brown is board-certified general surgeon, Certified by The American Board of Surgery, with a special interest in breast health. She is a member of the prestigious American College of Surgeons, Society of Surgical Oncology and The American Society of Breast Surgeons.

Dr. James H. Frost
MD, FACS, Physician
Dr. James Frost is a board-certified general surgeon, Certified by The American Board of Surgery, with a special interest in treating patients with benign and malignant breast disease. At Trinitas Hospital, Dr. Frost spearheaded the development of the multi-specialty breast cancer panel.

Dr. Desiree D’Angelo
MD, FACS, Physician
Dr. Desiree D’Angelo-Donovan is a board-certified general surgeon, Certified by The American Board of Surgery, who also specializes in the care of breast cancer and breast-related diseases. She has obtained special certifications from The American Society of Breast Surgeons.

Dr. Ann Chuang
MD, FACS, Physician
Dr. Ann Chuang is a fellowship-trained breast surgeon, Certified by The American Board of Surgery, with a special interest in breast health, benign breast disease and breast cancer.e has been named a Top Doctor in New York Magazine, Castle Connolly and Inside New Jersey magazine.

Dr. Lisa Iucci
DO, Physician
Dr. Lisa Iucci is a general surgeon with a special interest in treating breast diseases and skin cancer. She is board-certified by the American Osteopathic Board of Surgery. She is a member of the American Society of Breast Surgeons.

Dr. Vaishali Purohit
MD, Surgeon
Dr. Vaishali Purohit is a board-certified general surgeon with fellowship training in breast surgery. She treats the full spectrum of breast diseases, including benign breast disease such as breast pain, high-risk counseling, and malignant breast disease.
Frequently Asked Questions
If I have breast pain, does that mean I have cancer?
Usually breast cancer—unless it is quite advanced—is painless.
Breast pain may have multiple origins, including but not limited to: fibrocystic changes, cysts, infection, hormonal cycle, trauma, dietary factors, inflammation from external sources, etc.
If you have breast pain, it is a good idea to consult your breast physician for a workup, diagnosis and treatment.
If my mother had breast cancer, does that mean that I will get breast cancer?
Only 5 percent of all breast cancers are related to pathologic genes (i.e., BRCA, amongst other pathologic genes).
However, your family history can put you in a higher risk group for breast cancer.
If you have a family history of breast cancer, you should consult your breast physician for a discussion of the appropriate screening modalities available to you.
I had an abnormality on my mammogram/ultrasound and received a call back for further imaging, does that mean that I have breast cancer?
Most breast callbacks are for further diagnostic views and imaging by other modalities and usually result in clarification of the question by imaging alone. Some imaging abnormalities will require biopsy. Most of these can be done with a needle and do not require open surgery. Most breast biopsies will yield benign, noncancerous results (80 percent or more).
If my recent breast biopsy shows cancer, will I need my breast removed?
The current treatment of breast cancer is multimodality, involving surgery (breast and plastics), medications (chemotherapy, hormonal therapy, immunotherapy) and radiation (e.g., whole breast vs. partial breast). Treatment recommendations will be discussed based on your personal history, risk assessment, the type, size, and location of the breast cancer you have, your personal habits and your preferences.
Two patients with the exact same breast cancer may elect for treatments at different ends of the treatment spectrum. For example, Patient A with a 2 cm tumor in the upper outer quadrant of her 34C breast may elect for breast conservation and radiation with post-op hormonal therapy. Meanwhile, Patient B with the exact same breast size, tumor size, type and location may elect to have both breasts removed, reconstructed and forego radiation and future imaging. Though these two treatments will yield equal outcomes, each treatment was the correct treatment for the individual patient.
If I have cancer in one breast, do I need to have the other breast removed?
Current data does not support routine contralateral prophylactic mastectomy (CPM) in normal risk individuals. Fear of getting breast cancer in the opposite breast is the least well-supported reason for having the normal breast removed (i.e., the surgical risks of having the breast removed and reconstructed are greater than the risks of getting cancer in that breast). In fact, unless you have personal risk factors that increase your risk of breast cancer in the normal breast, current research suggests that it may actually be detrimental to your overall health to have routine CPM.
Of course, a thorough discussion of risks, benefits and alternatives should occur with your breast surgeon prior to any breast cancer surgery. In some patients, who do not have a higher biologic risk, CPM may be the right choice for them because of other non-medical factors.
If I feel a lump, is it cancer?
It is a very good idea to get to know your breasts. A monthly self-exam can make you feel more comfortable with the makeup and appearance of your breasts, but more importantly will allow you to know if something is new (i.e., it wasn’t there before). Most lumps are benign, especially if they have a history and are non-changing. However, new and growing lumps warrant a visit to your breast physician and should usually be investigated.
What are the signs of breast cancer?
There isn't one specific sign of breast cancer. However, there are a constellation of findings that should warrant a trip to the breast physician. Such signs include, but are not limited, to changing lump, new/changing swelling or edema of the skin, an ulcerating skin wound, retraction (pulling in) of the skin, a change of breast shape, new nipple discharge, a new crusty appearance to the nipple/areola, a new lump in the armpit.
Do I need a breast MRI?
Most women do not require a screening breast magnetic resonance imaging (MRI) scan. These are usually reserved for high-risk women (lifetime calculated risk over 20 percent), and/or women who had a biopsy showing a high-risk lesion (e.g. atypical hyperplasia, lobular carcinoma in situ).
Breast MRIs are indicated in some breast cancer patients before surgery to exclude disease in the opposite breast and to evaluate the extent of disease in the affected breast. The decision for a breast MRI will usually be made after discussion with your physician and is usually based on your personal risk factors, your age and the type of breast cancer you have.
Breast MRIs are frequently performed for individuals receiving chemotherapy or hormone therapy before surgery to gauge the response of the tumor to therapy.
What lifestyle changes can I make to reduce my risk of breast cancer?
Family history and the chromosomes (genes) we receive from our parents are risk factors that we currently cannot change, though splicing and repairing pathologic genes may become available in the not-too-distant future.
Risks that the individual can control include:
- Fat cells in women produce extra estrogen hormone.
- How much is too much is still being debated. However, most experts agree that alcohol can increase breast cancer risk incrementally.
- Not only can smoking increase your risk of getting breast cancer, but smokers with breast cancer may do worse than non-smokers with breast cancer.
- Hormone therapy. Hormones, like estrogen, can increase risk of breast cancer. The risk is related to the length of time used and seems to decrease with time once the hormones are stopped.
Should I be worried if I have a nipple discharge?
In some women, nipple discharge can be associated with breast manipulation and/or hormonal changes. This is especially true if the same discharge is present in both breasts.
Most nipple discharge will be from a benign etiology.
A new, spontaneous, unilateral nipple discharge should initiate a visit with your breast physician.
What does the term “sentinel lymph node” refer to?
1) Selective estrogen receptor modulators:
- Tamoxifen: Original hormone treatment for breast cancer and can be used in premenopausal women.
- Raloxifene: Primarily used for osteoporosis and may reduce risk of certain breast cancers in high-risk individuals. The main risks include blood clot, uterine cancer and menopausal symptoms.
2) Aromatase inhibitors:
- Anastrozole, Exemestane: These drugs have been shown to effectively reduce risk of breast cancer in post-menopausal women.
The risks include osteoporosis, bone pain/muscle cramps and menopausal symptoms.
Margins (How much is enough?)
Current data does not support routine contralateral prophylactic mastectomy (CPM) in normal risk individuals. Fear of getting breast cancer in the opposite breast is the least well-supported reason for having the normal breast removed (i.e., the surgical risks of having the breast removed and reconstructed are greater than the risks of getting cancer in that breast). In fact, unless you have personal risk factors that increase your risk of breast cancer in the normal breast, current research suggests that it may actually be detrimental to your overall health to have routine CPM.
Of course, a thorough discussion of risks, benefits and alternatives should occur with your breast surgeon prior to any breast cancer surgery. In some patients, who do not have a higher biologic risk, CPM may be the right choice for them because of other non-medical factors.
What is Ductal Carcinoma in Situ?
Breast cancer cells are seen, but they are still inside of the breast ducts. They are noninvasive. This is felt to represent a pre-cancer or Stage 0 (The horse is still in the barn).
Ductal Carcinoma is graded (1-3). The higher the grade, the more aggressive it can be.
When diagnosed by needle biopsy, it requires further investigation, as it may be associated with invasive cancer.
We can be contacted during normal business hours, Monday through Friday from 9:00 A.M. to 5:00 P.M. Please call us directly to schedule an appointment. All urgent appointments will be scheduled as soon as the doctor has availability.
Only 5 percent of all breast cancers are related to pathologic genes (i.e., BRCA, amongst other pathologic genes). However, your family history can put you in a higher risk group for breast cancer. If you have a family history of breast cancer, you should consult your breast physician for a discussion of the appropriate screening modalities available to you.
How soon after my appointment can a surgical procedure be scheduled?
Generally, two weeks, depending on the type of procedure.
Where will my surgical procedure be performed?
Minor surgical procedures may be performed in the office setting or at a surgery center. For more complex procedures, they are typically scheduled at one of our affiliated hospitals.
Do the physicians perform laparoscopic procedures?
Absolutely! Several procedures can be performed laparoscopically with minimally invasive techniques.
If I have breast pain, does that mean I have cancer?
Only 5 percent of all breast cancers are related to pathologic genes (i.e., BRCA, amongst other pathologic genes). However, your family history can put you in a higher risk group for breast cancer. If you have a family history of breast cancer, you should consult your breast physician for a discussion of the appropriate screening modalities available to you.
How long will I be out of work after surgery?
It will depend on the type of surgery. For minor procedures, time off from work may not be required. For abdominal surgeries, there are lifting restrictions after surgery so it may be anywhere from 4 to 8 weeks. If your job involves heavy lifting and your employer does not offer "light duty," you may need to be out of work during that period of time. Our office will help with filling out FMLA or short-term disability paperwork, as needed.
Does someone have to drive me home after surgery?
If you are not having anesthesia, then you can drive yourself home.
If you are receiving anesthesia of any type (general, twilight, sedation, etc.) a responsible adult (over 18) will have to drive you home. You cannot take public transportation, taxi, or Uber/Lyft home after having anesthesia.
If I have breast pain, does that mean I have cancer?
Only 5 percent of all breast cancers are related to pathologic genes (i.e., BRCA, amongst other pathologic genes). However, your family history can put you in a higher risk group for breast cancer. If you have a family history of breast cancer, you should consult your breast physician for a discussion of the appropriate screening modalities available to you.
If I have cancer in one breast, do I need to have the other breast removed?
Current data does not support routine contralateral prophylactic mastectomy (CPM) in normal risk individuals. Fear of getting breast cancer in the opposite breast is the least well-supported reason for having the normal breast removed (i.e., the surgical risks of having the breast removed and reconstructed are greater than the risks of getting cancer in that breast). In fact, unless you have personal risk factors that increase your risk of breast cancer in the normal breast, current research suggests that it may actually be detrimental to your overall health to have routine CPM.
Of course, a thorough discussion of risks, benefits and alternatives should occur with your breast surgeon prior to any breast cancer surgery. In some patients, who do not have a higher biologic risk, CPM may be the right choice for them because of other non-medical factors.

